St. Pete Location
Bradenton Location
Patient Education
We're passionate about helping people achieve their healthiest, happiest skin. Whether you're struggling with acne, eczema, rosacea, or any other skin concern, we're here to offer support, information, and inspiration.
Early Stage Discoid Eczema: Signs, Causes & Treatment
Early Stage Discoid Eczema: What It Looks Like and What to Do Next
If you've noticed small, coin-shaped patches of red, itchy, or scaly skin appearing on your arms, legs, or torso, you may be experiencing early stage discoid eczema — also called nummular eczema or nummular dermatitis. While the name may sound unfamiliar, this chronic skin condition is more common than most people realize, and catching it early makes a significant difference in how quickly and effectively it can be managed.
At My Skin in St. Petersburg and Bradenton, Florida, our board-certified dermatology team sees patients with discoid eczema at all stages. This guide will help you understand the early warning signs, causes, triggers, and proven treatments — so you can take action before the condition worsens.
What Is Discoid Eczema?
Discoid eczema is a type of chronic inflammatory skin condition characterized by round or oval-shaped lesions on the skin. Unlike other forms of eczema (such as atopic dermatitis, which often appears in skin folds), discoid eczema appears as distinct, coin-like spots — hence the name "nummular," from the Latin word for coin.
It is classified as a form of medical dermatology because it requires accurate diagnosis and ongoing clinical management to prevent flare-ups and skin damage.
Who Is Most at Risk?
Discoid eczema can affect people of any age, but it is most commonly seen in:
Middle-aged and older adults (though it can occur in children and young adults)
Men between the ages of 55–65
Women in their teens and twenties
Individuals with dry skin or a history of other eczema types
People with a history of contact dermatitis, venous insufficiency, or skin infections
Early Stage Discoid Eczema: Signs and Symptoms
Recognizing early stage discoid eczema is critical because it is easiest to treat before the lesions multiply, spread, or become infected. Here is what to look for in the earliest phases:
1. Small, Round Red Patches
The first sign is usually a cluster of tiny red bumps or blisters that quickly form into a round, coin-sized patch. These patches can appear anywhere on the body, but are most frequently found on:
The lower legs and shins
The forearms and hands
The torso and back
Less commonly, the face or scalp
2. Intense Itching
The itching associated with discoid eczema can be severe and often worsens at night, interfering with sleep. In early stages, the urge to scratch is strong — and scratching can introduce bacteria, leading to secondary skin infections.
3. Oozing or Weeping Patches
Early lesions may ooze a clear or yellowish fluid, especially after scratching. This "weeping" is a sign of active inflammation and can increase the risk of infection if left untreated.
4. Scaly, Crusty Skin
As the initial blisters dry out, the patches often become covered with dry, scaly skin or a yellowish crust. The skin surrounding the patches may look reddish and irritated.
5. Skin That Looks Redder or Darker Than Surrounding Skin
Depending on your skin tone, the patches may appear red, pinkish, brown, or grayish. On darker skin tones, discoid eczema can sometimes be harder to detect early, which is why professional evaluation is so important.
What Causes Discoid Eczema?
The exact cause of discoid eczema is not fully understood, but research points to a combination of genetic, environmental, and skin barrier factors. Unlike some skin conditions, it is not contagious and cannot be spread from person to person.
Common Triggers and Contributing Factors
Dry skin: A compromised skin barrier is the most common underlying factor.
Skin injury: Insect bites, cuts, burns, or minor abrasions can trigger a patch to develop.
Bacterial infections: Staphylococcus aureus on the skin may trigger or worsen flares.
Contact allergens: Reactions to metals (like nickel), fragrances, or preservatives in skincare products.
Venous insufficiency: Poor circulation in the legs can lead to discoid eczema on the lower limbs.
Cold, dry weather: Florida's air conditioning season can be surprisingly dehydrating to the skin.
Stress: Emotional stress can trigger or worsen eczema flares in susceptible individuals.
Certain medications: Interferons, statins, and some topical products have been associated with flares.
How Is Discoid Eczema Diagnosed?
Because discoid eczema can mimic other skin conditions — including ringworm (tinea corporis), psoriasis, contact dermatitis, and even early-stage skin cancer — a professional diagnosis is essential. Self-treating without a confirmed diagnosis can delay proper care and even worsen symptoms.
At My Skin, our dermatology provider Leah Michel, APRN FNP-BC conducts a thorough skin examination. In some cases, she may perform a skin swab to test for bacterial infection, patch testing to identify contact allergens, or a skin biopsy if the diagnosis is unclear.
Our appointments are 30 minutes — longer than the industry average — because we believe in taking the time to truly listen, evaluate, and create a personalized treatment plan that works for your unique skin and lifestyle.
Early Stage Discoid Eczema Treatment Options
The good news: when caught early, discoid eczema typically responds very well to treatment. The goal is to relieve itching, reduce inflammation, heal the skin barrier, and prevent future flares.
1. Topical Corticosteroids
The first-line treatment for most discoid eczema cases. Prescription-strength steroid creams or ointments reduce inflammation quickly and help clear patches. Over-the-counter hydrocortisone is usually not strong enough for established patches.
2. Topical Calcineurin Inhibitors
Non-steroid alternatives such as tacrolimus (Protopic) or pimecrolimus (Elidel) are particularly useful for sensitive areas or when steroid use needs to be minimized.
3. Medicated Moisturizers and Emollients
Aggressive skin hydration is foundational to managing eczema. We may recommend medical-grade moisturizers to restore the skin barrier and prevent moisture loss — especially important in Florida where air conditioning can strip the skin.
4. Antibiotic Treatment (If Infected)
If a bacterial infection (most commonly Staphylococcus aureus) is present, oral or topical antibiotics may be prescribed alongside steroid treatment.
5. Antihistamines
Oral antihistamines can help control nighttime itching and allow for better sleep during active flares.
6. Phototherapy (Light Therapy)
For persistent or widespread discoid eczema that does not respond to topical treatments, narrowband UVB phototherapy is an effective option that reduces inflammation throughout the skin.
7. Lifestyle and Trigger Management
Identifying and avoiding your personal triggers is critical to long-term control. This includes:
Using fragrance-free, hypoallergenic skincare and laundry products
Wearing cotton clothing to minimize skin irritation
Taking lukewarm (not hot) showers and patting skin dry gently
Applying moisturizer immediately after bathing to lock in moisture
Keeping skin protected in cold, dry conditions
Discoid Eczema vs. Other Skin Conditions: How to Tell the Difference
One of the most important reasons to seek professional care is that discoid eczema closely resembles several other conditions. Here is a quick comparison:
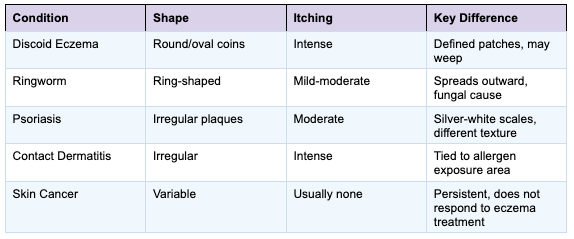
Because these conditions can look so similar, self-diagnosis and self-treatment is risky. A skin cancer examination or full skin check with our team can ensure that what you are seeing is correctly identified — and that nothing more serious is being missed.
When to See a Dermatology provider for Discoid Eczema
You should schedule an appointment if:
You notice new round, itchy, or scaly patches on your skin
Over-the-counter treatments have not improved your symptoms within 1–2 weeks
The patches are spreading, multiplying, or becoming more inflamed
You see signs of infection: increased redness, warmth, swelling, or yellow/green discharge
The itching is disrupting your sleep or daily activities
You are unsure whether what you have is eczema, ringworm, psoriasis, or something else
You have previously had discoid eczema and are experiencing a new flare
Living with Discoid Eczema: Long-Term Management Tips
Discoid eczema is a chronic condition for many patients, meaning flares can return — especially with seasonal changes or stress. However, with the right management strategy, most people achieve excellent control.
Daily Skin Care Routine
Moisturize twice daily with a thick, fragrance-free cream or ointment (not lotion)
Use lukewarm water for bathing; avoid long hot showers
Apply prescribed topical medications exactly as directed, even when skin looks clear
Protect skin from cuts, scrapes, and insect bites which can trigger new patches
Monitor and Avoid Your Triggers
Keep a simple skin diary to track when flares occur and what may have triggered them — a new soap, a stressful week, or a change in the weather. Sharing this with your dermatology provider helps fine-tune your treatment plan over time.
Frequently Asked Questions About Discoid Eczema
Is discoid eczema curable?
There is no permanent cure, but it is highly manageable. Many patients experience long periods of remission with proper treatment and skin care. Some people do have just one episode that clears and never returns.
Is discoid eczema contagious?
No. Discoid eczema is not contagious. It is an inflammatory skin condition related to your immune system and skin barrier, not an infection that can be spread through touch.
Can discoid eczema become infected?
Yes. Scratching the patches can introduce bacteria, most commonly Staphylococcus aureus, which can cause a secondary skin infection. Signs of infection include increased pain, warmth, swelling, yellow crusting, and red streaking. Seek care promptly if you notice these signs.
How long does a discoid eczema flare last?
Without treatment, flares can last for months. With appropriate treatment, many patients see significant improvement within a few weeks. Starting treatment early — ideally at the first sign of a new patch — leads to faster resolution.
Can children get discoid eczema?
Yes, although it is less common in children than in adults. Children who develop discoid eczema should be seen by a dermatology provider for accurate diagnosis and age-appropriate treatment.
Take the First Step Toward Clear, Healthy Skin
Don't let discoid eczema go undiagnosed or untreated. The sooner you seek professional care, the sooner you can find relief and protect your skin from further damage.
The information provided in this blog post is intended for educational purposes only and does not constitute medical advice, diagnosis, or treatment. The content is not a substitute for professional medical consultation, evaluation, or care from a qualified healthcare provider. If you are experiencing skin symptoms, please consult a licensed dermatology provider before beginning any treatment. Individual results may vary. At My Skin, Leah Michel, APRN FNP-BC develops personalized treatment plans based on each patient's unique medical history and skin needs. Always seek the advice of your physician or qualified health provider with any questions you may have regarding a medical condition. Do not disregard professional medical advice or delay seeking it because of something you have read on this website.
If you have any questions or concerns about your skin & would like to schedule an appointment at our St. Pete dermatology office or Brandenton dermatology office, please call us today!
St. Pete Location
111 2nd Ave NE., Suite 1406
St Petersburg, FL 33701
Plaza Tower- Downtown St Pete
Phone: (727) 295-7223








Mail
Facebook
LinkedIn
X