St. Pete Location
Bradenton Location
Patient Education
We're passionate about helping people achieve their healthiest, happiest skin. Whether you're struggling with acne, eczema, rosacea, or any other skin concern, we're here to offer support, information, and inspiration.
Acne Keloidalis Nuchae: Causes, Symptoms & Treatment
Acne Keloidalis Nuchae: Causes, Symptoms & Effective Treatments
If you've noticed small, itchy bumps forming at the back of your neck or lower scalp — bumps that seem to grow, harden, and won't go away — you may be dealing with a condition called acne keloidalis nuchae (AKN). Despite being relatively common, especially among men with curly or coarse hair, AKN is widely misunderstood and often left untreated until it causes lasting scars.
In this guide, we break down everything you need to know — from what causes AKN to the most effective treatment options available today.
What Is Acne Keloidalis Nuchae?
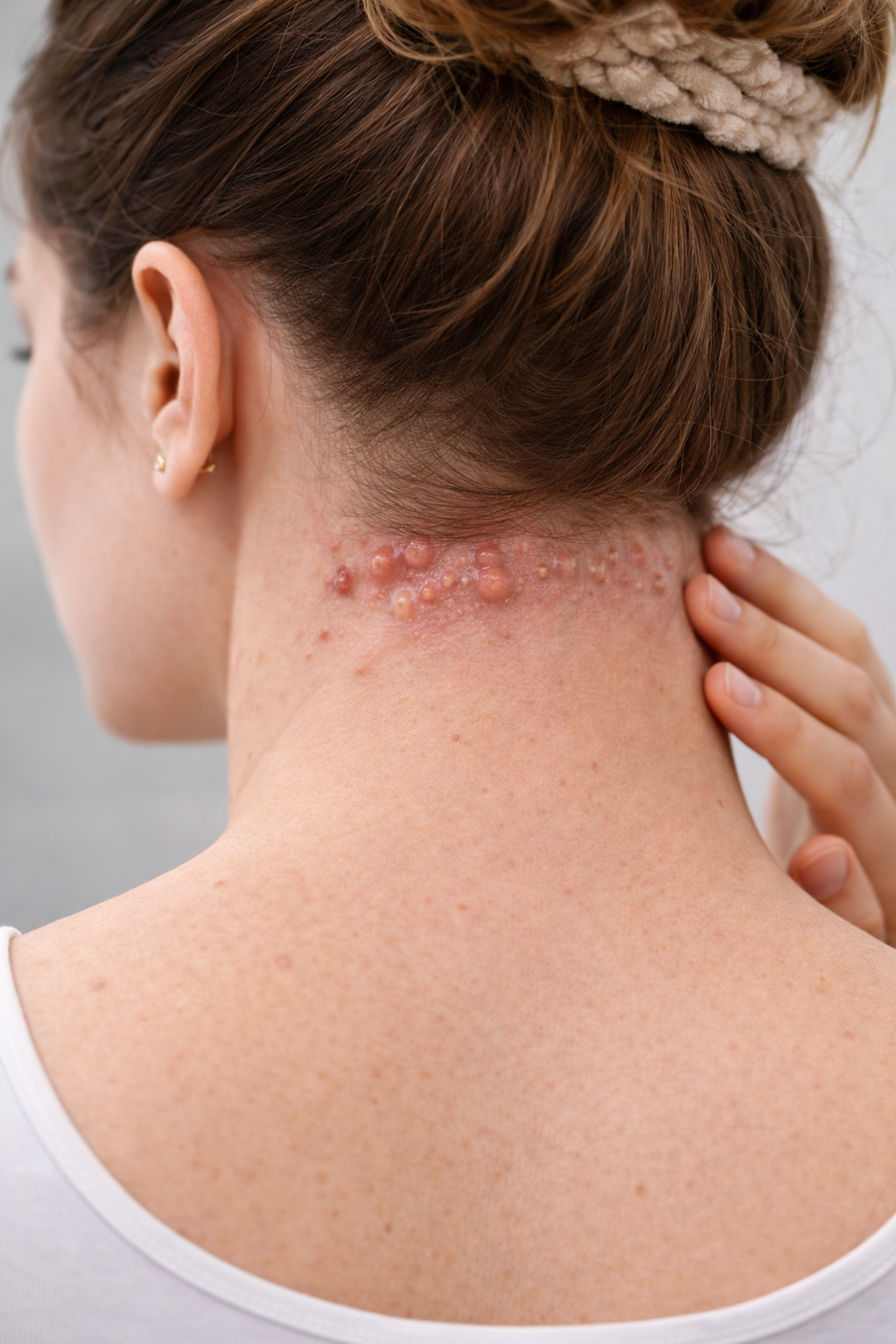
Acne keloidalis nuchae (AKN) is a chronic inflammatory skin condition that affects the hair follicles at the back of the scalp and the nape of the neck. Despite its name, AKN is not true acne, and the scars it produces are not technically true keloids. What's actually happening is a persistent folliculitis — inflammation of hair follicles — that leads to raised, keloid-like scar tissue if left untreated.
Over time, the small inflamed bumps (papules) can merge and enlarge into firm, thickened plaques. In advanced cases, AKN can cause permanent hair loss in the affected area — a condition called scarring alopecia. This makes early treatment critical to protecting your skin and hair long-term.
Also known as: folliculitis keloidalis, folliculitis keloidalis nuchae, keloidal folliculitis, and dermatitis papillaris capillitia — all referring to the same chronic condition.
Who Gets Acne Keloidalis Nuchae?
AKN most commonly affects postpubertal males, typically between the ages of 14 and 25. It is significantly more prevalent in men than women — at a ratio of approximately 20 to 1 — and disproportionately affects men of African descent, though it has been reported in Hispanic, Asian, and white individuals as well.
Individuals with darkly pigmented skin and those with curly, coarse, or tightly coiled hair are at the highest risk. However, AKN can develop in people with all hair types.
Causes & Risk Factors
AKN develops through a combination of chronic irritation, follicular trauma, and an exaggerated inflammatory response. Key contributing factors include:
Close or razor shaving: Short haircuts and razor shaving at the nape of the neck are among the most common triggers. Sharp, curved hairs re-enter the skin and provoke acute follicular inflammation.
Friction & irritation: Helmets, high-collared shirts, tight headwear, and athletic gear that rub against the back of the neck continuously traumatize hair follicles.
Bacterial or fungal infection: Bacterial overgrowth or Demodex mite infection may trigger or worsen follicular inflammation in susceptible individuals.
Certain medications: Drugs like cyclosporine and some immunosuppressants have been associated with triggering or worsening AKN.
Heavy hair products: Hair greases and pomades can clog follicles and aggravate inflammation in the affected area.
Androgens & seborrhea: Excess androgens or increased sensitivity to them, along with seborrhea, may contribute to follicular plugging and chronic inflammation.
AKN has also been associated with metabolic syndrome, obesity, hypertension, hidradenitis suppurativa, and hypothyroidism.
Symptoms to Watch For
AKN typically begins subtly and worsens gradually if untreated:
Stage 1 — Early: Small, Itchy Papules
Small red or skin-colored bumps appear at the back of the scalp and nape of the neck. They may be itchy or mildly tender. Many people mistake these for razor bumps or regular acne.
Stage 2 — Intermediate: Pustules & Plaques
Papules become pus-filled (pustules) and begin to cluster together, forming thickened raised plaques. The area becomes more painful and inflamed.
Stage 3 — Advanced: Scarring & Hair Loss
Without treatment, chronic inflammation leads to dense fibrosis and keloid-like scarring. Permanent hair loss (scarring alopecia) forms along the hairline. In severe cases, painful abscesses may develop.
Important: AKN will not resolve on its own. The longer it goes untreated, the greater the risk of permanent scarring and hair loss. Early intervention dramatically improves outcomes.
How AKN Is Diagnosed
A provider can typically diagnose AKN through a thorough physical examination of your neck and scalp. She'll review your hair care habits, clothing, and any prior treatments. If needed, they may also recommend:
Skin biopsy: A small tissue sample examined under a microscope for definitive diagnosis.
Bacterial or fungal culture: To identify infectious organisms that may be driving the inflammation.
Treatment Options
There is currently no single cure for AKN, but a range of highly effective treatments can manage the condition, reduce inflammation, prevent further scarring, and achieve significant long-term improvement. Treatment is tailored to the severity and stage of the condition.
1. Topical Therapies (Mild-to-Moderate AKN)
Topical antibiotics (clindamycin, erythromycin) — reduce bacterial colonization and inflammation
Topical corticosteroids (clobetasol, betamethasone) — calm the inflammatory response and reduce bump size
Topical retinoids (tretinoin) — promote cell turnover and prevent follicular plugging
Keratolytic agents (salicylic acid, AHAs) — soften and reduce papules
Antimicrobial cleansers (benzoyl peroxide wash, chlorhexidine) — reduce secondary infection risk
2. Oral Antibiotics (Moderate AKN)
Oral antibiotics such as doxycycline, minocycline, or tetracycline are prescribed for their anti-inflammatory and antimicrobial properties — especially helpful when pustules or active infection are present.
3. Intralesional Steroid Injections
Injections of triamcinolone acetonide directly into lesions can reduce bump size, soften hardened tissue, and calm deep inflammation. Administered every 2–3 weeks by your provider. Topical lidocaine may be applied beforehand for comfort.
4. Laser Therapy
Nd:YAG laser and diode laser — laser hair removal in the affected area to reduce new lesion triggers
Long-pulsed alexandrite laser — significant improvement shown in clinical studies
Erbium:YAG laser — demonstrated success treating AKN papules and plaques
5. Surgical Excision
For advanced or treatment-resistant AKN with large plaques or abscesses, surgical excision may be the most appropriate option. The My Skin Surgical Dermatology team uses minimally invasive techniques to minimize recurrence and scarring. Learn more at myskinstpete.com/surgical-dermatology.
6. Follicular Unit Excision (FUE)
A newer technique using small precise punches to extract affected follicles one by one. Recent research has shown promising long-term remission results for papular AKN cases.
Prevention & Self-Care Tips
Avoid close shaving: Skip razor shaving at the nape of the neck. Clipper cuts that leave some length are far less irritating to hair follicles.
Choose loose collars: Avoid tight-fitting shirts, turtlenecks, and athletic gear that rubs against the back of the neck.
Cleanse regularly: Use a gentle antimicrobial cleanser or medicated shampoo on the affected area daily.
Don't pick or scratch: Manipulating bumps worsens inflammation and dramatically increases scarring risk.
Avoid heavy hair products: Hair greases and pomades can clog follicles — opt for lighter, water-based products.
Seek care early: At the first sign of persistent bumps, consult a dermatology provider to prevent irreversible damage.
Frequently Asked Questions
Q: Is there a cure for AKN?
A: There is currently no definitive cure, but with the right treatment approach, symptoms can be effectively managed and many patients achieve long-term remission.
Q: Can AKN go away on its own?
A: No. AKN is a chronic, progressive condition that worsens without treatment, potentially leading to permanent scarring and hair loss.
Q: Is AKN contagious?
A: No. AKN is not contagious. It is a chronic inflammatory skin disorder, not an infectious disease.
Q: Can women get AKN?
A: Yes, though it is far more common in men. Women can develop AKN and still require professional evaluation and individualized treatment.
Q: Does insurance cover AKN treatment?
A: As a medical skin condition, AKN treatment is typically covered by insurance.
Schedule Your Appointment Today
Don't let acne keloidalis nuchae progress to permanent scarring. Leah Michel, APRN, FNP-BC at My Skin offers personalized, evidence-based treatment at our St. Petersburg and Bradenton locations.
Book online: myskinstpete.com/book-dermatology-appointment
St. Pete: (727) 295-7223 | 111 2nd Ave NE, Suite 1406, St. Petersburg, FL 33701
Bradenton: (941) 330-5805 | 4301 32nd St. W., Suite D2, Bradenton, FL 34277
Medical Dermatology: myskinstpete.com/medical-dermatology
Surgical Dermatology: myskinstpete.com/surgical-dermatology
Acne Treatment: myskinstpete.com/patient-education/b/acne
Meet Leah Michel: myskinstpete.com/meet-our-dermatology-provider-leah-michel
Disclaimer
This article is for informational purposes only and does not constitute medical advice. Please consult a qualified provider for diagnosis and personalized treatment recommendations.
If you have any questions or concerns about your skin & would like to schedule an appointment at our St. Pete dermatology office or Brandenton dermatology office, please call us today!
St. Pete Location
111 2nd Ave NE., Suite 1406
St Petersburg, FL 33701
Plaza Tower- Downtown St Pete
Phone: (727) 295-7223








Mail
Facebook
LinkedIn
X